WHO’s Quality of Care for Maternal and Newborn Health and Implementation Frameworks:
The WHO defines Respectful Maternity Care as “care that is organized for and provided to all women in a manner that maintains their dignity, privacy and confidentiality, ensures freedom from harm and mistreatment, and enables informed choice and continuous support during labor and childbirth” (WHO recommendations: intrapartum care for a positive childbirth experience, 2018). In its quality of care framework for maternal and newborn health, the WHO stresses the importance of both the provision and the experience of care. According to this framework, the provision of care has three subcategories (evidence based practices for routine care and management of complications, actionable information systems, and functional referral systems), and the experience of care has three subcategories (effective communication, respect and dignity, and emotional support). Improving the experience of care through respectful and people-centered maternity care practices is essential for increasing the utilization of childbirth facilities--one of the most effective ways to decrease maternal and infant mortality worldwide. In order to improve the provision and experience of care, the WHO outlines an implementation framework that strikes the necessary balance between “conformity to the evidence-based practices and accommodating contextual differences” (Quality of Care for Pregnant Women and Newborns, 2015). The framework includes seven important steps to improve quality of care: (1) establish a leadership group, (2) situational analysis/assessment, (3) adapt standards of care, (4) identify interventions, (5) implement interventions, (6) measure quality and outcomes, and (7) refine strategies. If we focus on improving both the provision of care and the experience of care using the WHO’s quality of care and implementation frameworks, we will create health care systems that are safe, effective, timely, efficient, equitable, and people‐centred--ultimately leading to the highest attainable quality of care, birthing facility utilization, and maternal and newborn survival rates.
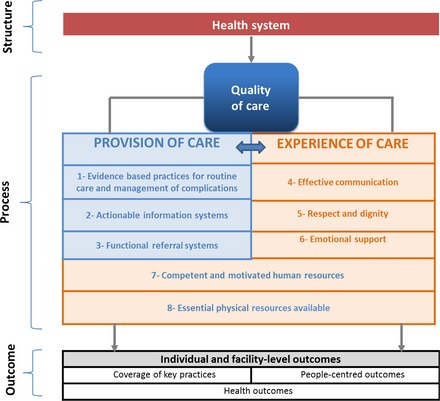
Credit: WHO's Quality of Care Framework for maternal and newborn health
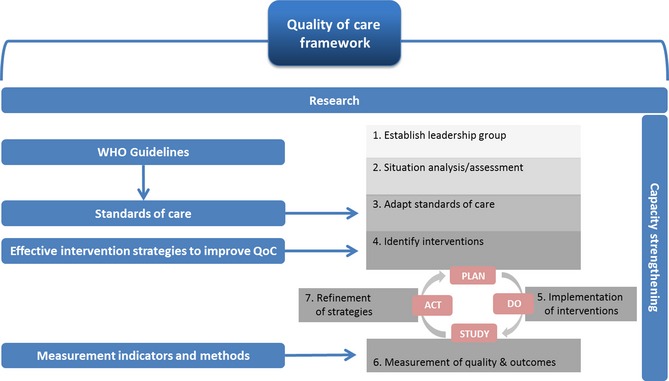
Credit: WHO's Implementation Framework
Person-Centered Maternity Care (PCMC) Scale:
The PCMC Scale is a universal framework for measuring PCMC in facility-based childbirth. It was developed using “literature and expert reviews to assess content validity, cognitive interviews with women to evaluate wording and appropriateness of the items, and psychometric analysis using survey data to assess construct and criterion validity and reliability” (Afulani 2019). The PCMC Scale has been proven valid and reliable for use in Low-Income and Middle-Income countries globally, allowing us to compare PCMC indicators across multiple settings for the first time. The PCMC Scale consists of three subcategories--dignity and respect, communication and autonomy, and supportive care--and includes 30 questions total. There is a mix of subjective and partly objective questions, each with answer options on a scale of 0-3; 0 means “no, never,” 1 means “yes, a few times,” 2 means “yes, most of the time,” and 3 means “yes, all the time.” The overall PCMC score is calculated by adding together the scores from each of the three subcategories; the lowest score possible is 0, and the highest is 90. The higher the score, the better the PCMC.

Credit: Measuring Person Centered Maternity Care for Women of Color (Afulani)
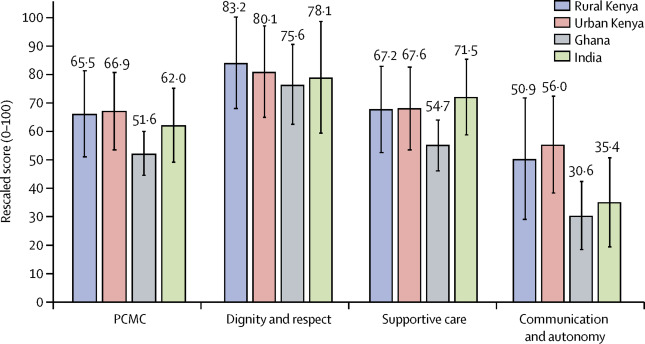
Credit: Person-centred maternity care in low-income and middle-income countries: analysis of data from Kenya, Ghana, and India (Afulani)

